Picture a highly controlled, medical-grade vacuum cleaner designed just for wounds. That's the simplest way to think about Negative Pressure Wound Therapy (NPWT), a powerful technique used to help complex or stubborn wounds heal faster.
You might also hear it called vacuum-assisted closure (or V.A.C. therapy), but the principle is the same. The system applies gentle, sub-atmospheric pressure to a wound, creating the perfect environment for your body's own repair mechanisms to kick into high gear. This advanced therapy has become a cornerstone in modern medicine for managing wounds that are slow to heal, offering hope and accelerated recovery for patients dealing with a range of challenging conditions.
What Is Negative Pressure Wound Therapy Explained
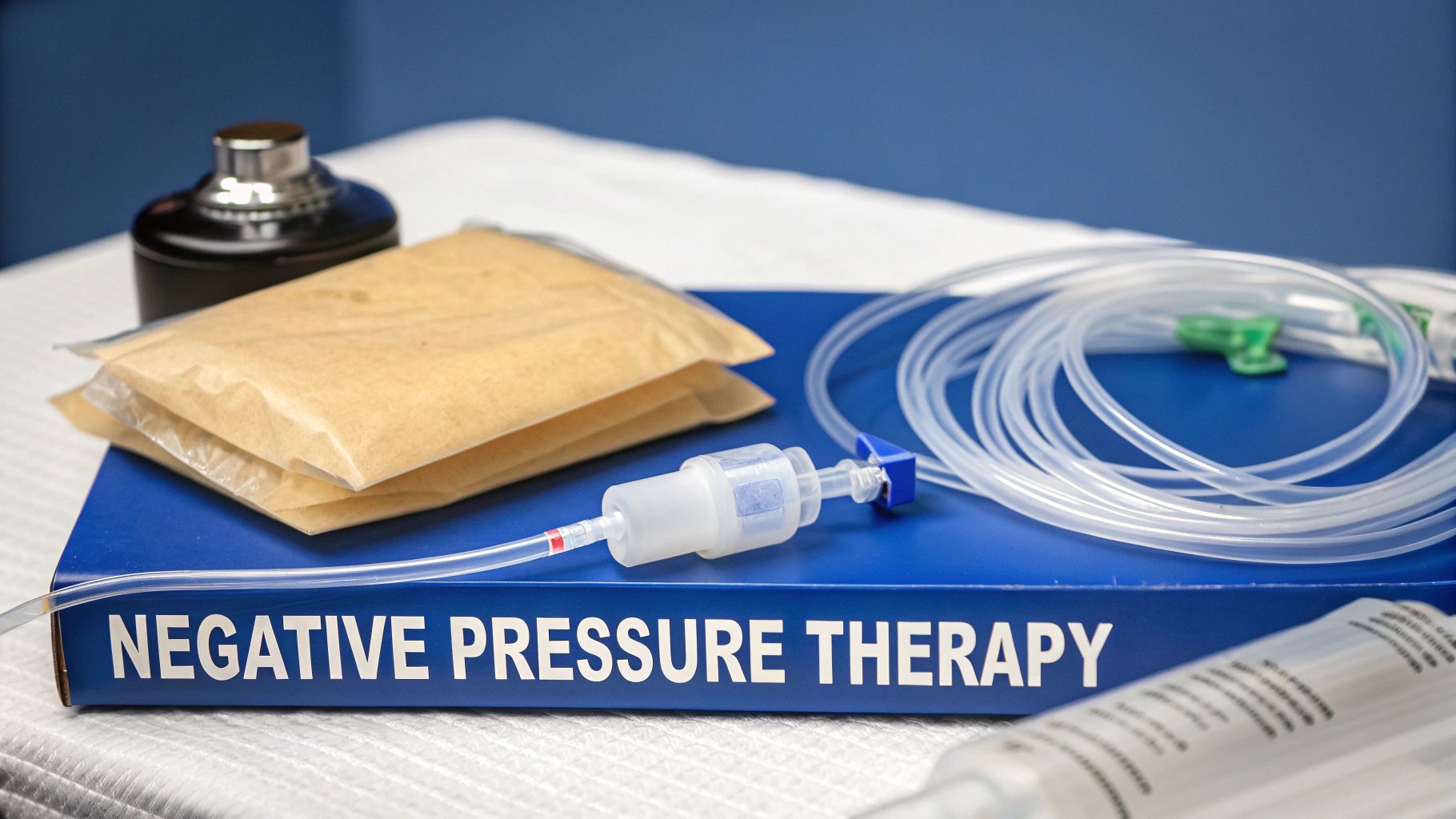
While the name sounds technical, the idea behind negative pressure wound therapy is refreshingly simple. This isn't just a passive bandage covering an injury; it's an active healing system. By applying controlled suction through a sealed dressing, the therapy physically draws wound edges together while encouraging the growth of fresh, healthy tissue. It transforms the wound bed from a passive, stagnant environment into a dynamic site of regeneration.
This modern approach to wound care has become a go-to tool in hospitals and clinics since it first emerged in the early 1990s. Drs. Louis Argenta and Michael Morykwas are credited with pioneering the first commercial system, which gained FDA approval in 1995 and has since been adopted worldwide for its impressive results. Its introduction marked a significant shift from passive wound covering to active wound management, fundamentally changing outcomes for patients with difficult-to-heal wounds.
At its core, NPWT applies controlled suction through a special foam dressing connected to a vacuum pump. This action pulls out excess fluid (exudate), cuts down on swelling (edema), and speeds up tissue formation in all kinds of difficult wounds, from chronic ulcers to acute injuries. For those interested in the detailed evolution of this technology, you can explore the history of NPWT to see how it has evolved over the decades.
The Three Core Components of NPWT
The whole system is easier to grasp when you break it down into its three main parts. Each piece has a specific, critical job in creating that ideal healing environment. The synergy between these components is what makes the therapy so effective.
For a quick overview, here’s a look at the key components and what they do.
NPWT At a Glance: Key Components and Functions
| Component | Description | Primary Function |
|---|---|---|
| Porous Dressing | A sterile foam or gauze material cut to fit the wound bed precisely. | Acts as the interface between the wound and the vacuum, ensuring even pressure distribution. |
| Transparent Sealing Film | An adhesive drape placed over the dressing and the surrounding healthy skin. | Creates an airtight seal, which is absolutely essential for maintaining negative pressure. |
| Computerized Vacuum Pump | A small, often portable pump connected to the dressing with tubing. | Generates, monitors, and maintains the prescribed suction level, pulling fluid into a collection canister. |
Each part works in concert with the others to transform a wound from a passive problem into an active healing site. The precision of each component is vital for the therapy's success.
Let's look a bit closer at each one:
- Porous Foam or Gauze Dressing: This soft, sterile material is the first thing to touch the wound. A clinician carefully cuts it to match the exact shape of the wound bed, ensuring the vacuum force is spread out evenly and doesn't concentrate on one spot. The open-pore structure of the foam is key to promoting granulation tissue growth.
- Transparent Sealing Film: Think of this as the "lid" that seals the whole system. This adhesive sheet goes over the foam and sticks to the healthy skin around the wound, creating an airtight environment. Without a good seal, the pump can't maintain the necessary negative pressure, rendering the therapy ineffective.
- Computerized Vacuum Pump: This is the brains of the operation. The small, portable pump connects to the dressing through a tube and does all the hard work—generating the suction, making sure it stays at the exact level prescribed by the doctor, and collecting all the drained fluid in a canister. Modern pumps often have alarms to alert clinicians if the seal is broken or the canister is full.
By actively pulling out fluid, shrinking localized swelling, and physically drawing the wound edges closer together, NPWT creates a clean, protected, and controlled space that gives the body’s natural healing process a massive boost.
This system effectively turns a challenging wound into a manageable healing project. By taking over the jobs of fluid removal and tissue stimulation, NPWT gives clinicians a powerful tool for wounds that would otherwise struggle to close, setting a new standard in advanced wound care. It is a proactive approach that doesn't just wait for healing but actively engineers the conditions necessary for it to occur.
How NPWT Works To Accelerate Healing
So, how does a sophisticated vacuum system actually convince a stubborn wound to heal? It's not just a fancy bandage. NPWT actively takes control of the wound environment, creating the perfect conditions for the body's natural repair crews to get to work. Its success lies in its multi-faceted approach, addressing several barriers to healing simultaneously.
The magic lies in four distinct but interconnected actions. Together, they clean the site, shrink the wound, and trigger new tissue growth from the inside out. Understanding these four pillars is key to seeing why this technology is a cornerstone of modern wound care.
Macro-Deformation: Pulling It All Together
The first and most obvious effect is macro-deformation. Think of it like pulling the drawstrings on a bag. When you pull, the opening cinches closed. NPWT does something very similar to the edges of a wound.
The gentle, continuous suction physically draws the wound edges toward the center. This mechanical force, also known as wound contracture, can shrink a wound's surface area by up to 80%, giving the body a much smaller, more manageable area to rebuild. It’s like giving your body a head start in the race to close the gap. This reduces the time needed for healing and can lead to less scarring.
Micro-Deformation: Signaling Cells to Grow
While macro-deformation works on the big picture, micro-deformation is happening at a cellular level. It’s a bit more subtle, but this is where the real regenerative power comes in. This process is often referred to as mechanotransduction—the conversion of mechanical stimuli into biochemical signals.
The specialized foam dressing that sits in the wound has a porous, textured surface. When the vacuum turns on, it gently pulls the wound tissue into these tiny pores. This creates a microscopic stretch on the individual cells—a mechanical signal that tells them it's time to divide and multiply (a process called cell proliferation). It's essentially a gentle workout that stimulates the growth of new, healthy granulation tissue, the bumpy, pink tissue that forms the foundation for new skin.
By creating both large-scale contraction and small-scale cellular stimulation, NPWT actively directs the body's repair processes. It doesn’t just wait for healing to happen; it encourages it at every level.
Fluid Removal and Environmental Control
The final two mechanisms work in tandem to turn a hostile wound environment into a pristine construction site for new tissue. A clean, balanced wound bed is a prerequisite for effective healing.
- Fluid Removal: Chronic wounds often weep excess fluid (called exudate), which is full of bacteria and enzymes that can break down healthy tissue and delay healing. NPWT acts like a sump pump, constantly pulling this harmful fluid away from the wound and into a collection canister. This reduces swelling (edema) and keeps the bacterial load low, creating a cleaner, healthier environment.
- Environmental Control: The clear film that creates the airtight seal is more than just a cover. It locks in moisture to prevent the new tissue from drying out while shielding it completely from outside contaminants and bacteria. This closed, protected, and moist space is the ideal incubator for healing, preventing infection and promoting cell migration across the wound bed.
By managing the wound environment so precisely, NPWT gives the body its best possible chance to heal efficiently. For those curious about how these same principles of fluid management and circulatory support apply in other wellness contexts, our article on how negative pressure supports circulation offers a deeper look.
Who Benefits From Negative Pressure Wound Therapy
Negative pressure wound therapy is a powerful tool in modern medicine, but it’s certainly not a one-size-fits-all fix. It’s specifically designed for those tough, complex wounds that just refuse to heal on their own. For these challenging cases, NPWT can be a game-changer, creating the perfect environment for the body to do its healing work.
This therapy is something a healthcare professional prescribes after taking a close look at the wound and the patient's overall health status. Getting the patient selection right is absolutely critical for success. The treatment works best in specific clinical situations where its unique actions—pulling out fluid, contracting the tissue, and stimulating new cells—can make the biggest difference.
Treating Chronic Non-Healing Wounds
Chronic wounds are injuries that get "stuck" in one of the healing phases, often the inflammatory phase, and can't move through the normal healing stages. This often happens because of underlying health problems like diabetes, poor circulation, or prolonged pressure. This is where NPWT really shines, helping to break the cycle of non-healing.
It is especially effective for treating:
- Diabetic Foot Ulcers: A serious and all-too-common complication of diabetes, these ulcers can lead to severe infections and even amputation. NPWT helps by drawing fresh, oxygenated blood flow to the area (improving perfusion) and removing infectious fluid, giving the body a much-needed advantage to finally close the wound.
- Pressure Ulcers (Bedsores): For people with limited mobility, constant pressure can starve tissue of oxygen and cause it to break down. NPWT improves circulation to these damaged spots and physically pulls the wound edges closer, encouraging new, healthy granulation tissue to grow from the bottom up.
- Venous Stasis Ulcers: Caused by faulty veins in the legs that lead to blood pooling, these wounds often come with a lot of swelling and fluid leakage. NPWT’s ability to constantly draw away this excess fluid is crucial. It reduces swelling and creates a cleaner, more manageable wound bed for healing.
Accelerating Recovery for Acute and Surgical Wounds
NPWT isn't just for chronic problems. It also plays a huge role in managing fresh injuries and complicated post-surgery sites. By controlling the wound environment right from the start, it becomes an invaluable tool for preventing complications and getting patients back on their feet faster.
One of the most impressive statistics is NPWT's ability to boost healing rates by 50-70% in diabetic foot ulcers. When used early, it can even prevent 20-30% of lower limb amputations. In orthopedics, the principles of NPWT can slash post-surgical swelling by 40-60% within just 48 hours, showing just how powerful it is in acute care. You can review the research on NPWT’s effectiveness for more details.
Key applications include:
- Traumatic Injuries: For large, messy wounds from accidents (like open fractures or degloving injuries), NPWT can stabilize the area, clear out contaminants, and get the wound bed ready for surgical closure or skin grafts. It acts as a bridge to definitive surgical repair.
- Complex Surgical Wounds: After major operations, particularly in the abdomen, incisions can sometimes split open (a process called dehiscence). NPWT helps manage this scary complication by keeping infection at bay and encouraging the wound to close up securely, often avoiding the need for further surgery.
It's essential to understand that patient selection is a clinical decision. A healthcare provider must assess the wound, the patient's overall health, and any underlying conditions to determine if NPWT is the appropriate course of action.
This careful evaluation ensures the therapy is applied where it will do the most good, cementing its medical credibility. Understanding these uses helps clarify why its core ideas—like boosting circulation and managing fluid—are so effective. Many of these benefits are tied to the body's natural drainage systems, a topic you can explore further in our guide on the role of lymphatic drainage in holistic wellness.
The Step-by-Step NPWT Application Process

Sometimes the best way to understand a medical technology is to see it in action. While NPWT is a clinical procedure performed only by trained professionals, walking through the application process can really demystify how it works.
It’s a precise, multi-step method designed to turn an open wound into a perfectly sealed, controlled healing environment. Each step, from cleaning the wound bed to activating the suction, has a specific and critical purpose. Let’s break it down.
Step 1: Preparing the Wound Bed
Before any part of the device touches the patient, the wound itself needs to be meticulously prepared. You could argue this is the most important step of all, because the therapy’s success hinges on starting with a clean, viable wound bed.
A clinician will first cleanse the wound, usually with a sterile saline solution, to flush away any debris or bacteria. This is often followed by debridement—a process where any dead or unhealthy tissue (necrotic tissue) is carefully removed. You need a clean base for new, healthy tissue to grow, and this step makes that possible. Without proper debridement, the therapy cannot reach the healthy tissue it needs to stimulate.
Step 2: Applying the Specialized Dressing
With the wound clean, the special foam or gauze dressing is put in place. This isn’t like applying a simple bandage. The dressing is carefully cut and shaped to fit the exact contours of the wound cavity, leaving no gaps.
This custom fit is crucial for two big reasons:
- It makes sure the negative pressure is distributed evenly across the entire wound surface, preventing localized pressure points.
- It protects the healthy skin surrounding the wound (the periwound skin) from the direct force of the suction, which could cause maceration or breakdown.
This precision ensures the therapeutic power is concentrated exactly where it’s needed most—right on the tissues that are trying to heal.
Step 3: Sealing the Site Airtight
Once the dressing is perfectly positioned, the next job is to create an airtight seal. This is done by placing a large, clear adhesive film over the dressing and several inches of the surrounding healthy skin.
Think of it like creating a protective bubble over the entire area. The film’s transparency is a key feature, allowing clinicians to monitor the wound without ever breaking the seal. Without this airtight environment, the pump simply can't maintain the consistent sub-atmospheric pressure needed for the therapy to work. Achieving a perfect seal can sometimes be challenging in difficult anatomical locations, requiring skill and experience.
The methodical process of cleaning, fitting the dressing, and sealing the site transforms an open injury into a closed, controlled healing system. This protects the wound from external contaminants while enabling the therapy to actively manage the internal environment.
Step 4: Connecting the System and Activating Therapy
The final steps are what bring the whole system to life. A small port or disc is attached to the adhesive film, which then connects to tubing that runs to the portable NPWT pump. This little port is the gateway for the negative pressure.
After everything is connected, the clinician programs the pump to the exact pressure level prescribed by the doctor—typically somewhere between -50 and -125 mmHg. The pump whirs on and starts pulling air from the dressing. You can see the foam dressing gently contract as it begins wicking away excess fluid.
Most patients describe the initial sensation as a light pulling or tugging. The therapy is now active, working 24/7 to manage fluid, reduce swelling, and kickstart tissue growth. The entire dressing is typically changed every 48 to 72 hours, and the process begins again. This regular change is necessary to assess the wound and prevent potential infection under the dressing.
Understanding the Risks and Contraindications of NPWT
While Negative Pressure Wound Therapy is a powerful tool for healing, it’s not the right solution for every wound. Just like any serious medical procedure, it comes with potential risks and a clear list of situations where it absolutely should not be used (contraindications).
Getting a clear-eyed view of these limitations is essential for patient safety and is a big part of what makes this a clinical therapy, not a general wellness device. Acknowledging the potential downsides helps everyone understand that NPWT is a prescribed treatment that demands a professional’s careful judgment and ongoing monitoring.
Potential Risks and Common Issues
Most of the issues that come up with NPWT are minor and manageable, but they require a healthcare professional to be watching closely. It’s important for patients to know what to look out for so they can flag any concerns for their care team right away.
Here are the most common risks:
- Discomfort During Dressing Changes: This is the most frequently reported issue. The foam dressing is typically changed every 48 to 72 hours, and some patients feel pain during this process as granulation tissue can grow into the foam. This is usually managed by giving pain medication before the dressing change begins or soaking the dressing with saline.
- Skin Irritation: The adhesive film used to create the airtight seal can sometimes bother the healthy skin around the wound, leading to redness, itching, or even blistering. Protecting the periwound skin is a key part of the application process.
- Infection: While NPWT is great at removing bacteria, if a wound is already badly infected before treatment starts, sealing it up could trap the infection and make things worse. This is why proper wound cleaning and debridement are non-negotiable first steps.
- Bleeding: In rare instances, the suction can disturb a fragile blood vessel or a clot, causing bleeding. This risk is a bit higher for patients who are on blood-thinning medications (anticoagulants). Close monitoring is essential.
When NPWT Must Be Avoided
More important than the manageable risks are the absolute contraindications—the scenarios where NPWT is simply too dangerous to use. A clinician must conduct a thorough assessment to make sure none of these red flags are present before even thinking about starting therapy.
NPWT is a powerful intervention, but its safe application depends entirely on correct patient selection. Applying this therapy in a contraindicated situation can lead to severe complications, underscoring the need for expert medical evaluation.
Here are the primary situations where NPWT is strictly off-limits:
- Malignancy in the Wound: If there is any cancerous tissue in the wound bed, NPWT is not an option. The therapy is designed to stimulate cell growth, and the last thing you want to do is encourage malignant cells to grow faster.
- Untreated Osteomyelitis: This is a serious bone infection. You can't put NPWT on a wound if the bone underneath is infected and that infection isn't being properly treated and brought under control. The therapy could mask the progression of the deep infection.
- Exposed Blood Vessels, Nerves, or Organs: Applying direct suction to these incredibly delicate structures can cause catastrophic damage or life-threatening bleeding. They must be completely covered or protected by tissue before NPWT can even be considered.
- Non-Enteric and Unexplored Fistulas: A fistula is an abnormal tunnel between two body parts. You should never apply NPWT to one until you know exactly where it goes, as the pressure could cause serious internal damage or fluid imbalances.
- Necrotic Tissue with Eschar: NPWT just doesn't work on wounds covered with thick, dry, dead tissue (eschar). The wound has to be properly debrided first to expose a healthy, viable tissue bed that the therapy can actually work on.
Understanding these boundaries is what makes NPWT a safe and effective medical tool. It highlights the critical difference between a prescribed clinical treatment for open wounds and non-medical technologies that use similar principles for wellness and recovery on intact skin.
The Evolution From Medical Treatment To Wellness Technology
It’s a familiar story in innovation: a powerful medical technology finds a new purpose in the world of wellness. The principles behind what is negative pressure wound therapy are a perfect example of this journey. The core idea—using controlled suction to boost the body's natural healing and circulatory functions—has been brilliantly adapted from a clinical treatment into a sophisticated wellness tool.
Think of it like the evolution of lasers. A powerful surgical laser is designed for precise, invasive medical procedures. Yet, the same core science inspired the development of gentle cosmetic lasers for skin rejuvenation. One is a highly targeted tool for a specific medical problem, while the other applies the same physics non-invasively to enhance overall health and appearance. The science is the same, but the application couldn't be more different.
Medical NPWT is specifically designed to heal open wounds by applying continuous negative pressure right at the site of damaged tissue. In stark contrast, wellness technologies inspired by this principle apply intermittent negative pressure to the outside of the body over healthy, intact skin, unlocking a whole new set of benefits for circulation, recovery, and aesthetics.
From Targeted Wound Repair To Systemic Enhancement
The fundamental difference comes down to the target and the method. Medical NPWT directs its power inward, pulling fluid out of a wound and drawing the edges of the tissue together to promote healing. It is a highly localized, intensive treatment for a specific pathology.
Wellness systems like the Vacustyler, on the other hand, use a gentle, rhythmic vacuum wave that envelops the entire lower body. This intermittent negative pressure acts like a powerful external pump for your circulatory and lymphatic systems. It creates a cyclical "push-and-pull" effect that revitalizes blood flow, mobilizes stagnant lymphatic fluid, and floods your muscles and skin with a fresh supply of oxygen and nutrients.
It’s the difference between using a specialized tool to fix a single broken pipe versus upgrading the entire plumbing system to improve flow and efficiency throughout the house. Both use pressure, but they solve different problems on a vastly different scale. One is remedial, the other is optimization.
Shared Benefits In Different Arenas
While the applications diverge, the underlying benefits of managing fluid and boosting circulation are universal. Both medical NPWT and its wellness counterparts are exceptional at reducing swelling and accelerating the body's natural recovery processes.
- In Medicine: NPWT reduces edema in a localized wound bed, which is crucial for helping new tissue form and preventing infection. This localized fluid management is key to preparing the wound for closure.
- In Wellness: Intermittent negative pressure works on a larger scale, reducing systemic swelling and fluid retention in the legs. This leads to that incredible feeling of lightness and helps speed up recovery after a tough workout by flushing metabolic waste products.
This shared scientific foundation is what makes the technology so reliable. For medspas and athletic departments, NPWT's proven ability to achieve edema reduction of up to 65% in lower extremities has clear parallels to non-medical vacuum therapies. The Vacustyler Avantgarde, for example, can produce immediate 25-35% circulation gains in just one 20-30 minute session. These effects are so significant they can help cut athlete recovery time by 40% post-training.
The transition from medical NPWT to wellness applications is a story of innovation. It’s about taking a proven scientific principle and re-imagining its potential, moving from treating injury to optimizing the body's natural systems for better performance, faster recovery, and enhanced aesthetics.
This evolution allows wellness professionals to offer services grounded in solid scientific principles. For those interested in the aesthetic applications, you can learn more about how this works in our guide on using vacuum therapy for cellulite. The result is a safe, non-invasive service that delivers tangible benefits, showing how a concept born in the hospital has found a new, powerful purpose in the world of modern wellness.
Common Questions About Negative Pressure Wound Therapy
As you get familiar with any advanced therapy, a few questions are bound to pop up. This is especially true when a medical concept inspires a wellness application. Let's clear up some of the most common queries about negative pressure therapy to round out your understanding.
Is Negative Pressure Wound Therapy Painful?
Most patients describe the feeling of medical NPWT as a gentle, constant pulling or tugging on the wound site, not sharp pain. The therapy itself is usually very well-tolerated.
The main point of discomfort, if any, tends to happen during dressing changes, which are typically scheduled every 48 to 72 hours. As new tissue grows, it can adhere to the foam dressing. Clinicians know this and will often provide pain medication beforehand to ensure the process is as smooth and comfortable as possible. Soaking the dressing with sterile saline before removal can also minimize discomfort.
Wellness devices inspired by this science, like the Vacustyler, are a completely different story. They apply intermittent negative pressure over healthy, intact skin and are designed to be a relaxing, painless, and often quite enjoyable experience.
How Long Does NPWT Treatment Usually Last?
There's no one-size-fits-all answer here. The duration of medical NPWT is tailored entirely to the specific wound and the patient's healing progress. A clinician will map out a timeline based on a few key factors.
- Wound Type: A clean, acute surgical wound might only need the therapy for a couple of days to get a head start on healing.
- Wound Size and Depth: Deeper, larger, or more complex wounds will naturally need a longer course of treatment to properly heal from the inside out.
- Patient's Overall Health: A person's general health and any underlying conditions (like diabetes or peripheral artery disease) can play a big role in how quickly their body responds and repairs tissue.
Treatment can be as short as a few days or extend to several weeks or even months for a stubborn, chronic wound. The goal is always the same: continue until the wound bed is healthy enough for surgical closure (like a skin graft) or has healed on its own.
What Is The Difference Between Medical NPWT and a Vacustyler?
This is a crucial distinction, particularly for professionals in the wellness, recovery, and aesthetics fields. While both technologies use the principle of negative pressure, their purpose, application, and mechanism are fundamentally different.
Medical NPWT is a clinical treatment for open wounds. It applies direct, sustained negative pressure into the wound bed to actively remove fluid, contract the wound, and stimulate the growth of new, healthy tissue. It's a targeted medical intervention for injury. It is invasive in the sense that it is applied directly to compromised tissue.
On the other hand, a wellness device like the Weyergans Vacustyler uses intermittent negative pressure on the outside of the body, over healthy skin. Its goal isn't to heal a specific wound but to support the body’s systemic circulatory and lymphatic functions. Think of it as the difference between a surgical tool and a full-body wellness system. It is completely non-invasive.
Can Anyone Use Negative Pressure Therapies?
Absolutely not, and this is a critical safety point for both medical and wellness applications.
Medical NPWT is a prescription-only treatment for patients with very specific types of wounds. It has strict contraindications and cannot be used in certain situations, such as over cancerous tissue, on untreated bone infections (osteomyelitis), or where major blood vessels are exposed in the wound bed. A thorough medical evaluation is mandatory.
Likewise, wellness systems that use intermittent negative pressure have their own set of contraindications. A person with an acute thrombosis (blood clot), severe, unstable heart conditions, active infections, or during pregnancy, for example, would not be a candidate. A thorough consultation is always the first step to ensure the therapy is both safe and appropriate for the individual.
Ready to see how the science of negative pressure can elevate your wellness or recovery services? Weyergans HighCare US offers the Vacustyler Avantgarde, a state-of-the-art system that applies these principles for non-invasive aesthetic and athletic recovery benefits. Discover how to enhance circulation, speed up recovery, and offer your clients a unique, science-backed experience by visiting https://weyerganshighcareus.com.


